Ovarian Cancer: The Importance of Early Diagnosis
Annie Allsopp, Clinical Trainer, Clinical Leadership Team, CBAT
Introduction
Ovarian cancer is the 6th most common cancer in women, with around 7,500 diagnoses each year, and is one of the most common gynaecological cancers that has the highest mortality rate.
Ovarian cancer begins when abnormal cells in and around the ovary and fallopian tubes grow and divide in an uncontrolled way and form a cancerous tumour (malignant). The cancerous cells grow into surrounding tissues and can spread to other parts of the body.
There are several different types of ovarian cancer and the type of cancer depends on the type of cell and tissue it starts in. The three main types of ovarian cancer start from three common cell types: Epithelial cells, which cover the outer layer of the ovary, Germ cells, which produce the eggs (ova) and Sex cord stomal cells, that provide structure to the ovary and produce hormones.
When ovarian cancer is diagnosed, the spread of the cancer will be determined. This is called staging. The stages are numbered 1-4 and these stages are further broken down into smaller groups, which describes the extent of the cancer, after viewing under a microscope. Ovarian cancer is also described by its grade. The grade defines how healthy the cancer cells appear and can help to predict how fast they are likely to grow and spread. Grade 1 describes cancer tissue that contains many healthy-looking cells, Grade 2 describes cancer tissue in which more cells appear abnormal than healthy and Grade 3 describes cancer tissue with a lack of normal structure in which more abnormal than healthy cells appear.
Treatment will depend upon the type, stage and grade of cancer and will also take into account the general health of the woman. As is the case with most cancers, the earlier the diagnosed, generally, the easier it is to treat.
Anatomy and Physiology
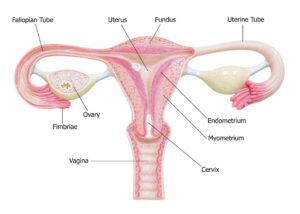
The ovaries are two small glands that form part of the female reproductive system, which is also made up of the vagina, cervix, uterus and fallopian tubes (Figure 1). They are solid structures, loosely held in place by peritoneal ligaments. They are located at each side of the uterus and are around the size and shape of an almond. The ovaries produce, store and release eggs for reproduction and are responsible for production of oestrogen and progesterone: hormones which play a key role in reproductive health. The ovaries consist of an outer cortex and an inner medulla, which is made up of loose connective tissue, blood vessels, lymphatic vessels and nerve fibres.
Figure 1. The Female Reproductive System (Image courtesy of Verywell Health)
Risk Factors
The most important risk factor for ovarian cancer is a family history of breast or ovarian cancer. Personal history of breast cancer is associated with an increase in the risk of ovarian cancer and ovarian cancer risk increases in women with a family history of breast, uterine, or ovarian cancer in their mother or sister.
Symptoms can be bloating, stomach pain, difficulty eating and frequency urinating. Back pain, changes in bowel habits, extreme tiredness or unexplained weight-loss may also be ovarian cancer symptoms. As a preventative strategy, an oophorectomy may be performed to remove the risk of the woman developing ovarian cancer. This is an operation to remove one of or both of the ovaries. The most common reason for having an oophorectomy is an ovarian cyst. It is also performed to treat problems such as a twisted ovary, which may occur when the cyst causes the ovary to swell. Symptoms are very similar with ovarian cysts and ovarian cancer and, therefore it is important for women to see their GP
at the earliest possible time.
Diagnosis
Diagnosis of ovarian cancer includes a rectovaginal pelvic examination, a transvaginal ultrasound, which is a scanning device inserted into the vagina, and a CA-125 blood test. CA125 is a protein made by some ovarian cancers, which circulates in the bloodstream. A biopsy of the tissue is the only clear way to determine ovarian cancer (Figure 2). Most women have a biopsy during a laparotomy, which is an operation performed under general anaesthetic to look inside the abdomen and pelvis. Tissue samples can be taken during this procedure. A laparoscopy, or keyhole surgery is less invasive and involves a small cut in the abdomen and a thin tube with a light and a camera, where the ovaries and surrounding area may be viewed and a sample taken for biopsy. Some women may be offered a guided biopsy instead, where a needle is inserted to take the biopsy. This is a procedure that is usually performed in the CT or ultrasound scanning room, under a local anaesthetic. This may not be possible if the cancer is in an area which is difficult to get to.
Tumour histology, age at diagnosis, body mass and smoking are also strongly linked with ovarian cancer survival, according to the analysis led by Oxford Population Health.
When a woman is diagnosed with ovarian cancer, they will be assigned to a multidisciplinary team (MDT) of gynaecological cancer specialists. This specialist oncology team overseeing treatment will usually include a gynaecological oncologist and a clinical nurse specialist (CNS).
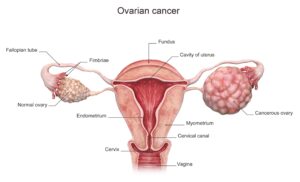
Figure 2. Comparison of a normal ovary to a cancerous ovary
Survival Rates
According to figures produced by Cancer Research UK, almost 15 out of 100 women will survive ovarian cancer for five years or more after they are diagnosed. However, survival rates often depend on many factors. For example; age, general health and co-morbidities. Regarding, the stage of cancer, there are no UK wide statistics available by stage, although there are statistics available for ovarian cancer in England by stage.
Almost 95% of women with Stage 1 will survive for 5 years or more following diagnosis, whereas, for Stage 2, survival rates drop to almost 70% for the same period after diagnosis. Figures show a survival rate of more than 25% for Stage 3, reducing to almost 15% survival rate for 5 years following diagnosis for Stage 4 (Figure 3)
The stage of cancer is related to the size and potential spread and the grade of cancer relates to the appearance of the cells microscopically (Figure 4). Both the type and grade as well as the woman’s general health and fitness will be predisposing factors which are likely to influence survival rates.
The Oxford Population Study highlighted that a key reason for poor survival is that many women are first diagnosed when they have advanced disease, while The Million Women Study highlighted that the more advanced tumours were associated with poor survival, those older at diagnosis, and those who reported higher body mass index (BMI) and smokers, had a worse survival rate.
Figure 3. Stages of ovarian cancer
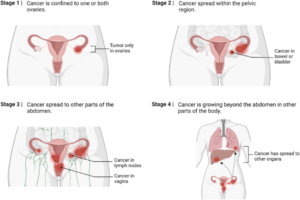
Figure 4. Grades of ovarian cancer
Treatment
The treatment plan will be discussed and determined according to the stage and type of ovarian cancer, with the aim of the treatment to cure the cancer or control it for as long as possible. A
treatment plan will be made following discussion, which will take into account, the type of cancer, stage and grade, the woman’s general health and their personal preferences. Advantages and
disadvantages will be conveyed by the health professional before a treatment plan is agreed.
Ovarian cancer is usually treated by a combination of surgery and chemotherapy and radiotherapy may be used to reduce symptoms. Chemotherapy is a drug treatment that uses powerful chemicals to kill fast-acting cells in the body, whilst radiotherapy is radiotherapy is a type of ionising radiation that destroys cancer cells in the treated area by damaging the DNA.
The aim of the surgery is to remove as much of the cancer as possible and to assess the extent of the disease. One or both ovaries may be removed and often, the uterus will be removed, depending upon the spread. This is called a hysterectomy. Lymph nodes may also be removed to assess if the cancer has spread. Chemotherapy may be given before surgery to shrink the cancer and after surgery to destroy any remaining cancerous cells. Hormonal therapy and radiotherapy may be recommended to improve symptoms. Cancer treatments can also cause early menopause and can affect fertility and this will also be considered in the treatment plan.
Ovarian cancer can return and can spread to other parts of the body. This is called metastasis. In metastasis, cancer cells break away from the primary tumour, travel through the blood or lymphatic system and form a new tumour in other organs or tissues. There is no single trajectory for ovarian cancer, but if not caught in the early stages, most cases will follow a similar path: from the pelvis to more distant parts of the abdomen and peritoneal cavity, to the lymph nodes and the liver. This may mean that the cancer cannot be cured but can be controlled with further surgery and chemotherapy for a considerable time.
Screening
A large study called UKCTOCS has looked at whether screening could be useful. Over 20,000 women took part, aged between 50 and 74 years old and data was collected and analysed between 2001 and 2020. The research study showed that ultrasound tests could not find ovarian cancers early or save lives, blood tests did detect cancers earlier, although this did not lead to saving lives either. Further research analysis is required from the data collected from the trial and the women continue to be screened. As a result of the trial, the NHS can not introduce a national screening programme using ultrasound or blood tests. The UK National screening Committee have agreed to review the longer term results when they are published.
Conclusion
Women have a higher risk of developing ovarian cancer if two or more of their relatives on the same side are diagnosed with ovarian or breast cancer at a young age, particularly under the age of fifty. It is recommended that women talk to their GP if they are at increased risk, where they may be referred to the genetic service for assessment and may be put on the UK Familial Ovarian Cancer Registry, which is a unique resource dedicated to advancing critical research necessary to find better ways to prevent, detect and treat ovarian cancer.
Clinical trials continue to gather data for ovarian cancers and recent significant breakthroughs for low grade serous cancer, whereby a new drug combination has demonstrated positive results in shrinking tumours, is encouraging. Whilst there is the additional positive news that new blood tests are in development and newfound proteins could aid in ovarian cancer detection, it is apparent that more research is needed to steer preventative strategies.
Early diagnosis of ovarian cancer holds the key for better outcomes from treatment plans and improved survival rates.
References
Cancer Research UK. https://www.cancerresearchuk.org (accessed 26 February 2024)
National Institute of Health, NCBI https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6500433/ (accessed 04 March 2024)
National Ovarian Cancer Coalition https://ovarian.org.uk (accessed 02 March 2024)
NHS Choices https://www.nhs.uk/conditions/ovarian-cancer/tests-and-next-steps (accessed 06 March 2024)
Target Ovarian Cancer https://target ovarian cancer.org.uk (accessed 08 March 2024)
Tobias J, Hochhauser D. Cancers and its management (7th edition) Blackwell J 2015
UKCTOCS, Ovarian cancer population screening and mortality after long-term follow-up in the UK Collaborative Trial of Cancer Screening: a randomised control trial Prof Usha Menon et al, published May 12, 2021
Yale Medicine https://www.yalemedicine.org/conditions/ovarian-torsion (accessed 14 March 2024